Articles
- Page Path
- HOME > J Educ Eval Health Prof > Volume 15; 2018 > Article
-
Brief report
Benefits of focus group discussions beyond online surveys in course evaluations by medical students in the United States: a qualitative study -
Katharina Brandl1*
 , Soniya V. Rabadia2
, Soniya V. Rabadia2 , Alexander Chang2
, Alexander Chang2 , Jess Mandel2
, Jess Mandel2
-
DOI: https://doi.org/10.3352/jeehp.2018.15.25
Published online: October 16, 2018
1Skaggs School of Pharmacy and Pharmaceutical Sciences, University of California San Diego, La Jolla, CA, USA
2School of Medicine, University of California San Diego, La Jolla, CA, USA
- *Corresponding email: kbrandl@ucsd.edu
© 2018, Korea Health Personnel Licensing Examination Institute
This is an open-access article distributed under the terms of the Creative Commons Attribution License <http://creativecommons.org/licenses/by/4.0/>, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
Abstract
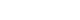
- In addition to online questionnaires, many medical schools use supplemental evaluation tools such as focus groups to evaluate their courses. Although some benefits of using focus groups in program evaluation have been described, it is unknown whether these inperson data collection methods provide sufficient additional information beyond online evaluations to justify them. In this study, we analyze recommendations gathered from student evaluation team (SET) focus group meetings and analyzed whether these items were captured in open-ended comments within the online evaluations. Our results indicate that online evaluations captured only 49% of the recommendations identified via SETs. Surveys to course directors identified that 74% of the recommendations exclusively identified via the SETs were implemented within their courses. Our results indicate that SET meetings provided information not easily captured in online evaluations and that these recommendations resulted in actual course changes.
- The UCSD Institutional Review Board designated this study as an EBP/QI/QA (evidence-based practice, quality improvement, and quality assurance) project and therefore did not require full review (IRB approval no., 151319QI).
- Analysis of the SET meeting notes yielded 69 suggested course improvements that included potential solutions, which were coded into the 7 categories listed earlier (Table 1). Of the 69 issues identified via SET, online evaluations captured 34 (49%). Specifically, SETs were superior in capturing feedback regarding specific teaching modalities in courses (18% appeared in online evaluations), problems related to the overall course content (25% online), and lecture content and organization (25% online). In contrast, online evaluations captured most of the deficiencies in study materials (80%), administrative course components (67%), exam-related problems (63%), and sequencing of course events (58%).
- Survey data from the course directors identified that 74% of the recommendations captured exclusively in SETs (in contrast to online evaluations) translated into course changes (26 of 35). Table 1 lists all suggested improvements and indicates whether each item was implemented by the course director and captured in the open-ended comments from the online evaluations.
- Evaluation is an integral part of medical education, and many tools are available to comprehensively characterize a program. One major purpose of collecting evaluations is to guide instructional improvement. Our analysis revealed that 74% of the SET-identified actionable items translated into course changes, implying that the focus groups served as a catalyst for discrete course adjustments. Studies have suggested that written comments may provide useful information that go beyond that of numerical ratings generated by closedended Likert-style questionnaires [7]. However, 2 major problems are associated with open-ended comments. First, interpreting students’ comments is not an easy task and there are no opportunities for asking clarifying questions. Second, open-ended comments often lack specificity and contextual factors [7]. Implementing a focus group as part of the evaluation process addresses both shortcomings. SET meetings facilitate negotiation, listening, and responding. Recommendations suggested by students in these meetings are discussed with faculty and deans in a collaborative dialogue. Students can explain proposed solutions and avoid confusion or misjudgments from faculty. In contrast to online open-ended comments, SET evaluations were rich in specific suggestions for improvement and also often included a contextual factor. Most importantly, our results indicate that suggestions identified in the SET meetings met the gold standard for evaluation comments—they actually led to course changes. The ‘give-and-take’ from multiple stakeholders in a course can best facilitate this process.
- No single evaluation tool will capture the entirety of all potentially useful feedback. The choice of an evaluation model should no longer be a treasure hunt for the one perfect evaluation model. It should be viewed as an ‘all of the above’ approach, rather than a ‘best single answer’ choice. Our data indicate that including open-ended focus groups can provide rich solution-based feedback that makes this a worthwhile tool to add to the evaluation toolbox.
Ethic statement
-
Authors’ contributions
Conceptualization: KB, SVR, AC, JM. Data acquisition: SVR, AC. Data analysis: KB, SVR, AC. Project administration: KB, JM. Writing–original draft: KB, JM. Writing–review & editing: KB, SVR, AC, JM.
-
Conflict of interest
No potential conflict of interest relevant to this article was reported.
-
Funding
None.
Article information
Acknowledgments
Supplementary materials
| Course | Actionable recommendations identified in SETs (by category) | Implementationa) | Captured in online evaluationsb) |
|---|---|---|---|
| Study materials | |||
| 1 | Implementing an additional practice quiz in a specific block. | Yes | No |
| 1 | Framing practice questions within clinical scenarios. | Yes | Yes |
| 1 | Improving the similarity of practice quiz questions and final exam questions. | Yes | Yes |
| 3 | Organizing practice quizzes by week regardless of the subject matter. | Yes | Yes |
| 3 | Including detailed explanations for the […] question on the practice quiz. | Yes | Yes |
| 4 | Increasing the number of practice quiz questions to ≥ 25. | Some | No |
| 4 | Providing practice quizzes as PDFs as well as on the online exam software. | No | Yes |
| 4 | Specifying the relevant lecture within each practice quiz question explanation. | Some | Yes |
| 6 | Increasing the resolution of specific images on the practice quizzes. | Yes | Yes |
| 7 | Adding more practice questions to a specific course syllabus. | Yes | Yes |
| Sequencing of events/coordinating events | |||
| 1 | Adjusting the scheduling of a patient presentation that includes difficult psychosocial interactions and sensitive topics to allow adequate time for reflection. | No | No |
| 1 | Adjusting the schedule to provide any integrative reviews of a complex topic immediately after that topic’s presentation in lecture, rather than at the end of the course. | Some | Yes |
| 2 | Adjusting the schedule to provide a full day for processing between a complex topic presented in lecture and small group exercises on the same topic. | Yes | Yes |
| 3 | Improving coordination between the physical exam in the practice of medicine course with the corresponding material in the relevant block. | Yes | No |
| 3 | Ensuring that diseases presented in clinical skills sessions are described in lectures prior to those sessions. | Some | No |
| 3 | Adjusting the schedule to prevent the placement of a flipped lecture onto a lecture-heavy day, especially if the following day includes TBL on that material. | Some | Yes |
| 4 | Improving the scheduling of the laboratory sessions. | Yes | No |
| 5 | Adjusting the schedule to avoid 4-hour lecture blocks the day before the final exam. | Yes | Yes |
| 6 | Ensuring that conditions presented in case studies sessions are described in lectures prior to those sessions. | Yes | Yes |
| 6 | Adjusting the lecture schedule to avoid presenting particularly complex and difficult concepts immediately before the final exam. | Yes | Yes |
| 8 | Scheduling all pathology lectures after the relevant pathophysiology lectures. | Some | No |
| 8 | Adjusting the lecture schedule to reflect the topic sequence within the recommended textbook of the course. | Some | Yes |
| Course (administrative component) | |||
| 1 | Posting of lecture notes beforehand to enable the students to download in time. | Yes | No |
| 1 | Clarifying the learning objectives on […]. | Yes | Yes |
| 1 | Improving the clarity of acronyms used in lectures and proofreading lecture notes for typos. | Some | Yes |
| 1 | Clarifying specific details on the drug list posted on the course website. | Some | Yes |
| 2 | Encouraging lecturers to maintain timing of lectures to 50 minutes. | Yes | Yes |
| 4 | Improving the correlation of the drug list with the lecture material. | Yes | Yes |
| 6 | Clarifying the relative importance of textbook material early in the course. | Yes | Yes |
| 6 | Requiring lecturers to finish within their allotted time. | Yes | Yes |
| 7 | Adding space on small group handout to allow annotations. | Yes | No |
| 7 | Posting the drug list for […] on the course website. | Yes | No |
| 8 | Focusing reports of negative performance to students rather than including deans and other administrators. | Yes | No |
| 8 | Providing clear expectations on textbook reading (supplemental versus required). | Some | Yes |
| Course content | |||
| 1 | Providing more emphasis for the importance of high-yield facts during the introduction lecture. | Yes | No |
| 1 | Adding an introductory lecture in a specific block. | Some | No |
| 2 | Adding definitions of […] to the lecture slides. | Yes | No |
| 2 | Include an integrative overview figure (favorite figure) to guide students to differentiate between different tests. | Yes | No |
| 2 | Adding organization to lectures and start with an important overview before adding details. | Some | Yes |
| 2 | Adding specific sessions within this course on how to write research papers. | Some | Yes |
| 3 | Adding the presentation of drugs into the […] lecture. | Some | No |
| 4 | Adding the discussion of specific diseases […] that are important for USMLE step 1. | Some | No |
| Exams | |||
| 2 | Providing calculators on computerized exams other than the calculator embedded in the exam software. | Yes | No |
| 3 | Adding more images to a specific portion of the exam. | Yes | Yes |
| 3 | Adding explanations to the […] portion in the exam review session. | Yes | Yes |
| 4 | Providing images with higher resolution on the computerized exam. | Some | No |
| 4 | Matching the difficulty of practice questions with actual exam questions. | Yes | Yes |
| 8 | Modifying the questions to reflect USMLE guidelines for multiple choice questions and increasing the use of clinical vignettes in question stems. | Yes | Yes |
| 8 | Ensuring that images used on the computerized exam are high-resolution. | Some | Yes |
| 9 | For each exam question that requires multiple lab values or a common clinical vignette, ensure that each question provides the needed information. | Yes | No |
| Lecture organization/content (specific lectures) | |||
| 1 | Increasing the emphasis of general concepts rather than small details in the […] lecture. | Yes | No |
| 1 | Matching the […] lecture content with the learning objectives. | Some | No |
| 3 | Adding more opportunities for interactive engagement and expanding on the pathophysiology of the […] lecture. | Yes | No |
| 3 | Improving the organization of the […] lecture. | Some | No |
| 3 | Eliminating duplicative material of the […] lecture. | No | Yes |
| 4 | Reducing the amount of slides in the […] lecture. | Yes | No |
| 5 | Reducing the research background in the […] lecture and increasing its clinical relevance. | Yes | No |
| 8 | Improving the organization for the […] lecture. | Yes | Yes |
| Specific teaching modalities | |||
| 1 | Providing PowerPoint summary slides for the small groups to minimize the impact of facilitator variability between the groups. | No | No |
| 2 | Assigning a specific time in the beginning of the small group exercise for students to review the paper. | No | Yes |
| 3 | For in-class problem-solving sessions, posting detailed answers immediately after class. | Yes | No |
| 3 | Increasing the interactive component of the […] sessions. | Yes | No |
| 4 | Changing teaching modalities (small group activities should be replaced by TBL sessions). | Some | Yes |
| 5 | Eliminating slides that only show pathologic tissues, rather providing slides with additional information. | No | No |
| 6 | For case study problems, ensuring that each problem is formatted so it can be used later as a practice question, by providing the question with the answer on the following slide. | Yes | No |
| 7 | Improving facilitator training to ensure that proper etiquette is enforced in all small group sessions. | Yes | No |
| 7 | Improving facilitator training to ensure each facilitator provides an adequate overview of the disorder and associated pharmacology. | Yes | No |
| 8 | Improving the case vignettes during the laboratory sessions. | Some | No |
| 9 | Adding detailed explanations to the small group. | No | No |
SET, student evaluation team; TBL, team-based learning; USMLE, United States Medical Licensing Examination.
a) Course directors revealed whether the suggested change was fully implemented (yes, n=41), somewhat implemented (some, n=21), or not implemented (no, n=7).
b) Actionable recommendations were captured (yes, n=34) or not captured (no, n=35) by open-ended comments from online evaluations.
- 1. Brandl K, Mandel J. What else is happening?: a more holistic view of programme evaluation. Med Educ 2018;52:352-354. https://doi.org/10.1111/medu.13524 ArticlePubMed
- 2. Colbert-Getz JM, Baumann S. Changing medical students’ perception of the evaluation culture: is it possible? J Educ Eval Health Prof 2016;13:8. https://doi.org/10.3352/jeehp.2016.13.8 ArticlePubMedPMCPDF
- 3. Koufakou A, Gosselin J, Guo D. Using data mining to extract knowledge from student evaluation comments in undergraduate courses. Proceedings of the 2016 International Joint Conference on Neural Networks (IJCNN); 2016 Jul 24-29; Vancouver, Canada. Piscataway (NJ). Institute of Electrical and Electronics Engineers2016. 3138-3142. Article
- 4. Uijtdehaage S, O’Neal C. A curious case of the phantom professor: mindless teaching evaluations by medical students. Med Educ 2015;49:928-932. https://doi.org/10.1111/medu.12647 ArticlePubMed
- 5. Brandl K, Mandel J, Winegarden B. Student evaluation team focus groups increase students’ satisfaction with the overall course evaluation process. Med Educ 2017;51:215-227. https://doi.org/10.1111/medu.13104 ArticlePubMed
- 6. Hsih KW, Iscoe MS, Lupton JR, Mains TE, Nayar SK, Orlando MS, Parzuchowski AS, Sabbagh MF, Schulz JC, Shenderov K, Simkin DJ, Vakili S, Vick JB, Xu T, Yin O, Goldberg HR. The Student Curriculum Review Team: how we catalyze curricular changes through a student-centered approach. Med Teach 2015;37:1008-1012. https://doi.org/10.3109/0142159X.2014.990877 ArticlePubMed
- 7. Alhija FN, Fresko B. Student evaluation of instruction: what can be learned from students’ written comments? Stud Educ Eval 2009;35:37-44. https://doi.org/10.1016/j.stueduc.2009.01.002 Article
References
Figure & Data
References
Citations

- Grupos focais como ferramenta de pesquisa qualitativa na fisioterapia: implicações e expectativas
Dartel Ferrari de Lima, Adelar Aparecido Sampaio
Revista Pesquisa Qualitativa.2023; 11(27): 361. CrossRef - Educational attainment for at-risk high school students: closing the gap
Karen Miner-Romanoff
SN Social Sciences.2023;[Epub] CrossRef - Student evaluations of teaching and the development of a comprehensive measure of teaching effectiveness for medical schools
Constantina Constantinou, Marjo Wijnen-Meijer
BMC Medical Education.2022;[Epub] CrossRef - National Security Law Education in Hong Kong: Qualitative Evaluation Based on the Perspective of the Students
Daniel T. L. Shek, Xiaoqin Zhu, Diya Dou, Xiang Li
International Journal of Environmental Research and Public Health.2022; 20(1): 553. CrossRef - Mentoring as a transformative experience
Wendy A. Hall, Sarah Liva
Mentoring & Tutoring: Partnership in Learning.2021; 29(1): 6. CrossRef

 KHPLEI
KHPLEI


 PubReader
PubReader ePub Link
ePub Link Cite
Cite